Pelvis
The human pelvis is a bony ring made of the sacrum in the back and the two innominate bones on the sides and in the front. There is no inherent stability to the pelvis and these three bones are held together by the strong sacro-iliac ligaments in the back, sacro-spinous and sacro-tuberous ligaments in the pelvic floor, and symphysis pubis in the front. These structures see a lot more load during daily activities than their strength can withstand suggesting that dynamic muscle forces protect them from injury during high intensity activities.
Each innominate bone is formed by fusion of the Ilium, pubis, and the ischium at the triradiate cartilage in the acetabulum. Damage to triradiate cartilage under 8 years can cause post-traumatic dysplasia, which is characterized by having a steep sourcil, wide ’V’ shaped tear drop, thick iliac part of the acetabulum, and relative retroversion (more posterior dysplasia than anterior with a cross over sign.). Triradiate cartilage fusion was discussed as a treatment option to correct protrusio acetabuli in children. Limbus (unossified lateral acetabulum and labrum complex) contributes to 30% of acetabular depth.
The posterior wall is not fully ossified till the triradiate cartilage closes. Apparent posterior wall deficiency (False cross-over sign) is seen on x-rays in 90 % of girls under 12 years of age and boys under14 years. Posterior wall fractures can be totally missed or their size underestimated on x-rays and CT. MRI is recommended after post traumatic hip dislocations in children.
Femoral head & Acetabulum influence each other’s development
Shape of the head determines shape of the acetabulum and vice versa. You probably heard of the experiment of placing a square object in the acetabulum and the acetabulum becoming square. An aspherical head as with Perthes, SCFE, and idiopathic cam with open triradiate cartilage makes the acetabulum wide anteriorly and laterally allowing the cam to enter farther. This seen as lateral joint space widening.
On the other head, a shallow acetabulum leaves the head aspherical with cam morphology while a deep acetabulum causes the head to be very round and the neck to be narrow. it is very common to see cam morphology with acetabular dysplasia probably from inadequate remodeling/rounding of the head because the socket was not deep enough to influence the head shape. Protrusio hips have a very spherical head with a narrow neck (low alpha angle). Protrusio and cam combination is less common and is very likely to become symptomatic early.
Pelvic incidence (PI)
The fixed structural relationship of the acetabulum to the sacrum is measured on the lateral view by the angle subtended between the line perpendicular to S1 end plate and another line connecting the centers of S1 end plate and the femoral head. PI is determined at birth and changes slightly during development. PI determines the position of the hips, pelvic tilt, shape of the butt, and spinal alignment. Theoretically, an anterior opening wedge innominate osteotomy can decrease the PI and a closing wedge osteotomy can increase the PI.
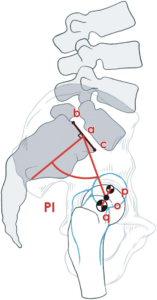
Acetabulum
The acetabulum is an incomplete cup in the innominate bone. The articular cartilage is inverted ‘U’ shaped, distributed in the front, back, and above the acetabular fossa. The acetabulum covers 70% of the femoral head. The acetabular fossa does not articulate with the femoral head. A high fossa decreases the medial extension of the articular cartilage in the dome of the acetabulum and decreases medial coverage of the femoral head. The insertion of the reflected head of the rectus femoris is at the top of the acetabulum, the so called 12 o’clock position. The mid anterior part of the acetabulum is where the iliopsoas tendon crosses the anterior wall, so called 3 o’clock position of the right hip. The acetabular wall is thin at 12 o’clock, thickens towards the AIIS and becomes thin again at 3 0’clock position. This morphology looks like a triangle and allows anterior rim trimming in the correct location without intraoperative fluoroscopy. The middle of the transverse acetabular ligament is at 6 o’clock position.
The anterior half of the acetabulum, along with the iliac crest above and the superior pubic ramus medially, constitutes the anterior column and the posterior half of the acetabulum, along with ilium extending to the SI joint above and the ischium below constitutes the posterior column. The thin medial wall of the acetabulum is called the quadrilateral plate.
Acetabular labrum is a fibrocartilaginous extension of the articular cartilage peripherally. A cleft between the articular cartilage and the labrum is normal posteriorly, but the labrum and cartilage are continuous on the anterior aspect. Hence, any disruption of the chondrolabral junction in the anterior aspect is considered pathological. The labrum increases the depth of the acetabulum and forms a suction seal around the head as it continues inferiorly as the transverse acetabular ligament. There isn’t any bone or cartilage next to the transverse acetabular ligament leaving a recess through which branches of the obturator nerve and artery enter the hip. Ligamentum teres originates from the transverse acetabular ligament and inserts into the fovea centralis on the femoral head. The labrum is separated from the hip capsule with a recess. So capsular stresses are not transmitted to the labrum. This recess fills up from scar formation or inflammation. The labrum has blood supply only on the outer aspect, but still heals well when repaired or reconstructed.
Muscles
There are 27 muscles that cross the hip joint. Gluteus medius is the primary abductor and its weakness causes a lateral lurch and increases the shear forces on the acetabular cartilage during walking. Gluteus maximus and hamstrings extend the hip and their weakness increases anterior pelvic tilt. Iliopsoas is the primary flexor of the hip and it can stabilize the hip from anterioriorly. Gluteus minimus is the primary internal rotator and is attached to the hip capsule. Hip adductors are quite strong and are thought to stabilize the hip in co-contraction with other groups of muscles.
Nerves
Superior gluteal nerve supplies the hip abductors and internal rotators and it is at risk from traction injury during posterior and lateral approaches as it passes anteriorly between gluteus medius and minimus from the top of sciatic notch to the front coursing 3-4 cm above the greater trochanter.
Femoral nerve courses on the antero medial aspect of Iliopsoas in the femoral triangle.
Sciatic nerve courses across the short external rotators of the hip posteriorly and is always superficial to the Quadratus femoris muscle.
Obturator nerve innervates the medial aspect of the hip and is thought also to cause referred pain from the hip to the knee.
Lateral femoral cutaneous nerve emerges from underneath the inguinal ligament close to the ASIS and passes superficially and laterally on the thigh. This is the most common nerve injury from anterior approach and anterior arthroscopic portals.
Blood supply to the hip joint
Lateral circumflex femoral artery supplies the anterior hip capsule and femoral neck. It does not contribute any blood supply to the femoral head directly or through any anastamosis.
Obturator artery supplies the medial capsule, acetabulum, ligamentum teres, and a small portion of the head around the fovea centralis. Not clinically significant to the head.
Lateral circumflex femoral artery supplies the anterior hip capsule and femoral neck. It does not contribute any blood supply to the femoral head directly or through any anastamosis.
Obturator artery supplies the medial capsule, acetabulum, ligamentum teres, and a small portion of the head around the fovea centralis. Not clinically significant to the head.
Medial circumflex artery arises in the femoral triangle anteriorly from profunda femoris or femoral artery, travels posteriorly over iliopsoas along the inferior border of obturator externus. Its deep branch gives rise to medial retinacular vessels that travel along the posterior aspect of medial synovial fold (ligament of Weitbrecht) to supply the inferior pat of the femoral head. Its ascending branch receives blood from the priformis branch of the inferior gluteal artery before it crosses over the obturator externus tendon and enters the hip capsule and courses up the neck in the lateral synovial fold. This lateral retinacular artery divides into 2-5 branches as they enter the femoral head at the articular cartilage border. These vessels can nourish the entire femoral head on their own even when all other blood supply is interrupted to the head. Disruption of these vessels cannot be compensated by any other supply to the head acutely. After physeal closure metaphyseal vessels may be able to supply the head in some hips with lateral vessel interruption. The piriformis branch anastomosis was the main source to lateral retinacular vessels in some hips. No other significant anastomosis contributes to femoral head blood supply.
The acetabulum is supplied by the superior gluteal artery on the lateral aspect, iliolumbar artery from the inner table, and obturator artery inferomedially with adequate flow possible from any one of these sources.
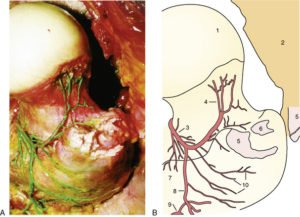
Reproduced from JBJS 2001. Ganz article
