The hip joint is between the femoral head (ball) and the acetabular socket in the pelvis (cup). Slipped Capital Femoral Epiphysis is a well known hip disorder in older children and adolescents. The ball slips through its growth cartilage and settles at an angle to the neck and the shaft.
Majority of slips happen in obese children without any other abnormality. Few patients may have hormonal disorders, renal disease, rickets etc.
Pain and limp are the most common complaints. The pain may be mild and felt in the hip, thigh, or the knee leading to delayed diagnosis. Children may continue to be active with some pain suggesting that the slip is stable. Untreated, the slip is likely to progress to a more severe degree either gradually or suddenly. Sudden exacerbation of the pain along with inability to walk even with crutches suggests an unstable slip, which has higher complications and poorer results. Patients can present with a fused slip causing pain and deformity after growth plate closure. These patients need treatment only for the residual deformity.
The diagnosis of the slip is usually suggested by the clinical exam and is confirmed by plain x-rays. A stable slip is not a dangerous condition and has few immediate complications as long as it does not become unstable. Unstable slip can develop serious problems with loss of blood supply to the slipped ball and result in arthritis. Both stable and instable slips change the shape of the femoral head and limit hip motion in certain directions. The more severe slips are well known to lead to arthritis and even the mild case can cause joint damage in the long term.
Treatment options
The goals of treating a slipped hip are to stabilize the slip from getting worse and avoid complications in the short term, correct the deformity and avoid joint damage in the long term. Once diagnosed with unstable or stable slip, the child is placed on rest and crutches, and surgery is recommended.
Dr. Prasad Gourineni from Amara Hip Preservation Center uses Internal rotation at 90 degrees of flexion (FIR) as a measure of the severity of anterior FAI in SCFE. It takes into account the slip morphology along with femoral antetorsion and acetabular morphology. Synovitis and pain will influence our exam and FIR under anesthesia is more reliable.
Type 1. FIR more than 10 degrees. In-situ screw fixation only.
Type 2 – FIR less than 10 but the projected alpha angle change from osteoplasty can increase FIR to 10. These get the screw and arthroscopic osteoplasty.
Type 3. FIR cannot be restored to 10 with the estimated alpha angle change from bumpectomy alone. These get a corrective osteotomy.
Dr. Gourineni chose 10 degrees as adequate FIR in SCFE children because they are usually obese and less active, and allowing natural remodeling of a small neck bump to get a few more degrees of FIR is acceptable compared to leaving a bigger bump to abrade against the labrum and acetabular cartilage with bigger deformities. 20 degrees should be the goal for active children.
In-situ screw fixation
A simple, quick procedure that involves a small incision and fixation of the femoral head in its place with a screw. This works well to freeze the head with the present deformity and has very few complications. The persistent deformity can cause damage to the joint. Dr. Gourineni developed and published on oblique screw fixation and recommends a fully threaded 7.3 mm cannulated screw.
Reshaping of the head and neck
The deformity caused by the slip acts as a bump and jams against the cup and its labrum causing damage. This bump can be easily removed through arthroscopic or limited open technique but it is adequate by itself only in mild slips. Dr. Gourineni published on his arthroscopic technique in a large series well before other authors have reported their experience.
Arthroscopy
We have a lot of experience with arthroscopic femoral neck osteoplasty and also performed arthroscopic femoral neck osteotomy and correction of the slip.
Osteotomy
In severe slips, in addition to the shaving of the bump, the ball has to be reoriented on the thighbone by separating the ball from the shaft called osteotomy. The reshaping and osteotomy can be done even after initial in-situ screw fixation.
The osteotomy can be done at several places below the ball. The farther down the osteotomy is performed from the ball, the more deformity is created at a second place to compensate for the head deformity. But the farther osteotomies are considered safer than an osteotomy close to the ball. Dr. Gourineni has vast experience with performing femoral neck osteotomy through surgical dislocation for all types of slips(See Figure B1 and Figure B2) and limited experience using the arthroscope. (See Figure F1, Figure F2 and Figure F3).
Femoral neck osteotomy with Surgical dislocation
Safe surgical dislocation of the hip joint while preserving the blood supply to the ball enables procedures that were once considered unsafe. The femoral head is separated from the neck completely at the area of the deformity, the neck is reshaped, and the ball is replaced on to the neck correcting the deformity completely.
This procedure involves a large incision, significant blood loss, and requires a high level of technical expertise. Incisions heal quickly in children, blood can be saved and given back, and several surgeons have performed the procedure safely.
This procedure is more readily accepted in unstable slips due to poor results with the other techniques, but fewer surgeons prefer this to other techniques in stable slips. This procedure has been safe in Dr. Gourineni’s hands and gave the best results in unstable slips and more severe stable and fused slips that cannot be corrected with osteoplasty.
Complications
All surgeries have complications. General complications from anesthesia, medical problems, infection, and healing issues are not in your surgeon’s control. Untoward damage to tissues, improper technique, and inadequate supervision of care are complications that can be avoided by the surgeon. In spite of the best efforts certain complications like avascular necrosis (loss of blood supply to the ball) and chondrolysis (deterioration of hip cartilage) can occur rarely after any hip procedure. A child’s and the caregiver’s inability to follow precautions can also lead to poor results.
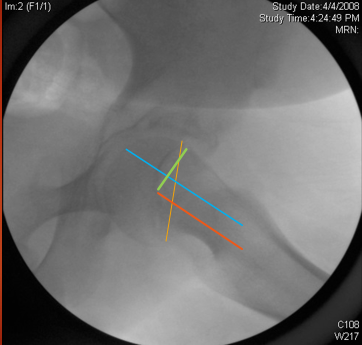
Analysis of slip deformity. Blue line is the neck axis. Red line is parallel to the neck axis and passing through the center of the head. Yellow line represents the physeal plane. Green line is from the center of the head to the Alpha point (point at which the head sphericity ends. Distance between the two blue and red lines is the amount of posterior translation. Angle between the green line and blue or red lines is the Alpha angle. Angle between the yellow line and red or blue lines is the posterior tilt of the head.
